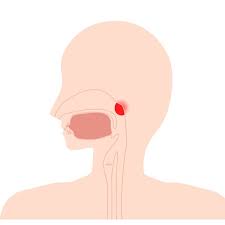
The term Adenoidid refers to the inflammation or infection of the adenoids, a small but significant mass of lymphatic tissue located at the back of the nasal cavity, near the roof of the throat. Although often overlooked, the adenoids play a vital role in the body’s immune system, particularly during early childhood, by helping to trap bacteria and viruses that enter through the nose and mouth. However, when these tissues become swollen or infected, they can cause a range of complications affecting breathing, sleep, speech, and overall quality of life. Adenoidid is most commonly seen in children, though it can occasionally persist or recur in adults.
The condition is frequently associated with symptoms such as nasal congestion, snoring, mouth breathing, and recurrent ear or sinus infections. It can develop as an isolated illness or as part of broader infections like tonsillitis or sinusitis. Despite being relatively common, many people fail to recognize the seriousness of untreated adenoid inflammation, which can lead to chronic respiratory issues, hearing problems, and even facial growth abnormalities in children.
In this extensive article, we will explore Adenoidid in detail—covering its anatomy, causes, symptoms, diagnosis, treatment options, and preventive care. We will also address how lifestyle, environmental factors, and modern medical innovations are influencing the management of adenoid conditions today. Whether you are a concerned parent, a medical student, or simply interested in understanding more about human health, this article offers a thorough and accessible guide to everything you need to know about adenoid inflammation.
1. Understanding the Role of Adenoids in the Human Body
To understand Adenoidid, it is essential first to grasp the function of adenoids themselves. The adenoids are part of the body’s lymphatic system, which is responsible for defending against infections and maintaining immune balance. Located in the nasopharynx—the area behind the nasal passages and above the soft palate—adenoids are made up of lymphoid tissue similar to that found in the tonsils. Together, the adenoids and tonsils form a protective ring known as Waldeyer’s ring, acting as the first line of defense against inhaled or ingested pathogens.
In children, the adenoids are relatively large because their immune systems are still developing and require strong barriers against new microorganisms. Over time, usually by adolescence, adenoids begin to shrink as the body builds a more mature immune response. However, during the period when they are most active, they can also become swollen or infected due to continuous exposure to bacteria and viruses. This overreaction leads to inflammation, congestion, and in some cases, chronic infection—resulting in the condition known as Adenoidid.
The adenoids are crucial during early years, but when inflamed, they can obstruct airflow through the nasal passages, leading to mouth breathing, snoring, and other respiratory complications. Thus, while adenoids serve an important function, their inflammation can paradoxically cause numerous health issues, particularly when left untreated.
2. Causes and Risk Factors of Adenoidid
There are several potential causes of Adenoidid, most of which are related to infections and environmental irritants. The most common cause is viral infection, particularly those caused by rhinoviruses, adenoviruses, and influenza viruses. These pathogens can enter through the nasal passages and trigger an immune response in the adenoid tissue. In some cases, bacterial infections—especially those caused by Streptococcus pneumoniae, Haemophilus influenzae, or Moraxella catarrhalis—can also lead to inflammation.
Children are particularly susceptible because of their still-developing immune systems and frequent exposure to pathogens in schools or daycare settings. Allergies can also contribute significantly to adenoid inflammation. When an allergic reaction occurs, the body’s immune response causes swelling in the nasal passages and surrounding lymphatic tissue, including the adenoids. Over time, chronic exposure to allergens like dust, pollen, or mold can lead to persistent adenoid hypertrophy (enlargement).
Environmental factors play a major role as well. Children exposed to cigarette smoke, pollution, or dry air are at higher risk for chronic nasal and adenoid irritation. Additionally, genetic predisposition can influence susceptibility to Adenoidid—families with histories of recurrent sinus infections, allergies, or tonsillitis may pass down this tendency. Lastly, immune system disorders or anatomical abnormalities can further complicate the condition, making some individuals more prone to chronic or recurrent adenoid inflammation.
3. Symptoms and Clinical Presentation of Adenoidid
The symptoms of Adenoidid can vary depending on the severity and duration of the inflammation. The most recognizable signs are nasal congestion, mouth breathing, and snoring. Because the swollen adenoids block airflow through the nasal passages, affected individuals—especially children—are often forced to breathe through their mouths, even during sleep. This can lead to a condition commonly referred to as “adenoidal facies”, where chronic mouth breathing alters facial growth and alignment, giving a characteristic long face and open-mouth posture.
Other common symptoms include frequent ear infections, difficulty swallowing, sore throat, and post-nasal drip. Adenoid swelling can also affect the function of the Eustachian tube, which connects the middle ear to the back of the throat. When this tube is blocked, it can lead to fluid buildup in the middle ear, resulting in ear pain, reduced hearing, and recurrent otitis media (middle ear infections).
In chronic cases, sleep disturbances such as obstructive sleep apnea may occur due to blocked airways. Children may show signs of restlessness, bedwetting, or poor academic performance caused by lack of restful sleep. Nasal speech—where the voice sounds congested or muffled—is another indicator of enlarged or infected adenoids.
Left untreated, Adenoidid can lead to chronic sinus infections, facial bone deformities, and even developmental issues in young children. Therefore, recognizing the early symptoms and seeking medical attention is crucial for effective management and prevention of long-term complications.
4. Diagnosis of Adenoidid
Diagnosing Adenoidid requires a combination of medical history, physical examination, and sometimes imaging or laboratory tests. A physician typically begins by asking about symptoms such as nasal obstruction, sleep disturbances, and ear problems. Because adenoids are not visible through a standard throat examination, doctors often use specialized instruments to visualize the area.
One common diagnostic tool is the nasopharyngoscope, a thin, flexible tube with a light and camera that allows direct visualization of the adenoid tissue through the nasal cavity. This procedure helps determine the size of the adenoids and whether inflammation or infection is present. In some cases, lateral neck X-rays are used to assess the degree of airway obstruction.
Laboratory tests, such as throat swabs or nasal cultures, may be performed to identify bacterial causes of infection. Allergy testing might also be recommended if chronic inflammation appears to be linked to allergic reactions.
In children experiencing chronic ear infections, audiometric testing (hearing tests) and tympanometry (middle ear pressure testing) are often used to evaluate whether enlarged adenoids are contributing to ear dysfunction.
Early and accurate diagnosis is essential for determining the most appropriate course of treatment, whether that involves medication, lifestyle changes, or surgical intervention.
5. Treatment Options for Adenoidid
The treatment of Adenoidid depends on the cause, severity, and frequency of the inflammation. In mild cases caused by viral infections, supportive care such as rest, hydration, and nasal saline sprays may be sufficient. Over-the-counter pain relievers and fever reducers can help manage discomfort.
For bacterial infections, antibiotics may be prescribed, although medical guidelines recommend caution to prevent antibiotic resistance. When allergies are the underlying cause, antihistamines, nasal corticosteroids, or immunotherapy may be used to control symptoms and prevent recurrence.
In cases of chronic or recurrent Adenoidid where conservative treatments fail, adenoidectomy—the surgical removal of the adenoids—may be recommended. This is a common and generally safe procedure, particularly in children who experience frequent ear infections, chronic sinusitis, or sleep apnea related to enlarged adenoids. Adenoidectomy often leads to significant improvements in breathing, sleep quality, and overall health.
Post-surgery care involves managing discomfort, preventing infection, and ensuring adequate hydration. Recovery typically takes about one to two weeks, with full return to normal activities shortly thereafter.
In modern medicine, newer minimally invasive techniques and the use of endoscopic guidance have made adenoid surgery safer and more precise, minimizing tissue damage and recovery time.
6. The Connection Between Adenoidid and Other Conditions
Adenoid inflammation rarely occurs in isolation; it is often associated with other health issues, particularly in the upper respiratory tract. One of the most common connections is between Adenoidid and Tonsillitis. Because the adenoids and tonsils are part of the same lymphatic network, infections in one area can easily spread to the other. Many children who suffer from chronic tonsillitis also have inflamed or enlarged adenoids, leading to the dual surgical procedure known as adenotonsillectomy.
Another frequent complication is Otitis Media with Effusion, also known as “glue ear.” When swollen adenoids block the Eustachian tubes, it causes fluid to accumulate in the middle ear, reducing hearing and increasing infection risk. Chronic adenoid inflammation may also contribute to sinusitis, as the blockage prevents proper drainage of nasal secretions.
In some cases, Adenoidid can exacerbate asthma or allergic rhinitis, as airway obstruction and mucus buildup trigger inflammatory responses throughout the respiratory system. Therefore, managing Adenoidid effectively requires a holistic approach that considers all interconnected systems and contributing factors.
7. Prevention and Lifestyle Management
Preventing Adenoidid involves maintaining strong immune health and minimizing exposure to infection and allergens. Good hygiene practices—such as regular handwashing, using clean tissues, and avoiding close contact with infected individuals—can greatly reduce the risk of viral or bacterial transmission.
For children, a balanced diet rich in vitamins A, C, and E helps strengthen immune defenses. Ensuring proper hydration and adequate sleep also supports natural healing mechanisms. Avoiding exposure to tobacco smoke, pollution, and dry indoor air is critical, as these irritants can inflame the nasal passages and adenoids.
Parents should also pay attention to early signs of nasal congestion, snoring, or recurrent ear infections in their children, as these may signal underlying adenoid issues. Regular pediatric checkups are essential, especially for children with a history of upper respiratory infections or allergies.
In environments where allergens are common, using air purifiers, washing bedding frequently, and keeping windows closed during high pollen seasons can make a significant difference. Ultimately, prevention focuses on creating a healthy environment that supports clear airways and reduces the frequency of infections.
8. Modern Advances and Future Directions in Adenoidid Treatment
In recent years, medical science has made remarkable advances in understanding and managing Adenoidid. Researchers are exploring biomarkers that can predict chronic adenoid inflammation and help doctors personalize treatment strategies. Imaging technologies such as high-resolution endoscopy and 3D imaging now provide more accurate assessments of adenoid size and function.
The use of laser-assisted adenoidectomy and radiofrequency ablation has revolutionized surgical treatment by offering minimally invasive options with less pain, faster recovery, and minimal bleeding. These innovations are particularly beneficial for pediatric patients, where reducing trauma and recovery time is a top priority.
Furthermore, the integration of AI and digital health tools is beginning to transform diagnosis and follow-up care. Mobile apps can now help track symptoms, breathing patterns, and sleep quality, allowing for better management of chronic adenoid-related conditions.
In the future, regenerative medicine and immunomodulatory therapies may play a role in restoring healthy adenoid function without surgery. Such advancements promise a future where Adenoidid can be treated effectively, safely, and with greater precision than ever before.
Frequently Asked Questions (FAQ)
Q1: What is Adenoidid?
Adenoidid refers to the inflammation or infection of the adenoids—lymphatic tissue located in the upper throat behind the nose—that can cause breathing difficulties, ear infections, and sleep disturbances.
Q2: Who is most at risk of developing Adenoidid?
Children between the ages of 2 and 10 are most susceptible due to their developing immune systems and frequent exposure to infections.
Q3: Can adults get Adenoidid?
Yes, although rare, adults can experience adenoid inflammation, often linked to chronic sinus infections or allergies.
Q4: What are the symptoms of Adenoidid?
Common symptoms include nasal blockage, mouth breathing, snoring, ear pain, sore throat, and recurrent respiratory infections.
Q5: How is Adenoidid treated?
Treatment may include antibiotics, nasal sprays, antihistamines, or surgical removal of the adenoids (adenoidectomy) in severe or recurrent cases.
Q6: Is Adenoidid contagious?
The condition itself is not contagious, but the viral or bacterial infections that cause it can spread from person to person.
Q7: Can Adenoidid be prevented?
Yes. Maintaining good hygiene, avoiding allergens and smoke, and supporting immune health can reduce the risk of inflammation.
Conclusion
Adenoidid is far more than a simple childhood condition—it represents a complex interaction between immunity, infection, and environmental influences. While often manageable with proper medical attention, untreated adenoid inflammation can lead to serious health complications that affect breathing, hearing, and overall development. Understanding its symptoms, causes, and treatment options empowers parents and patients to take proactive steps toward prevention and recovery.
Thanks to modern medical advancements, Adenoidid can now be diagnosed and treated more effectively than ever before. Whether through medication, lifestyle management, or surgery, early intervention remains the key to preserving health and well-being. In a broader sense, Adenoidid reminds us of the intricate balance within our immune systems and how maintaining that balance is essential to lifelong respiratory health.
By raising awareness, promoting preventive care, and embracing innovative medical approaches, we can ensure that Adenoidid is not only treated but ultimately controlled—allowing children and adults alike to breathe easier and live healthier lives.